COVID19
Associated Fire Fighters of Illinois
It is important to know that the around the clock the AFFI continues to gather information on this issue. If you need information on MOU’s, response plans, testing, vaccinations, CDC/IDPH guidance, or any other information, please communicate through your local’s President and then your AFFI District Vice President. For help finding information you can also contact Director of Health/Safety/ Education Drew Hansen at [email protected].
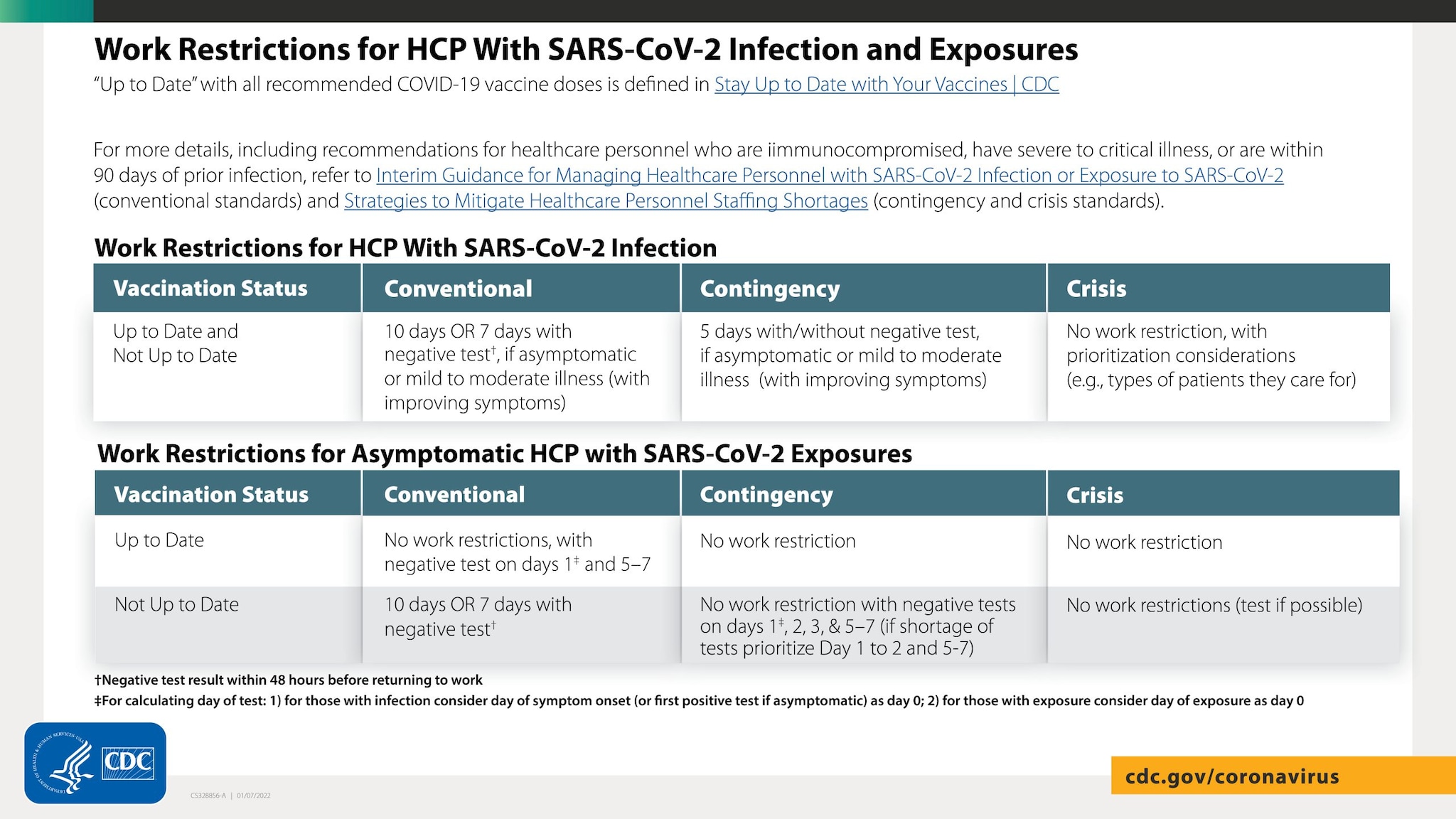
Updated CDC Guidance for HCP Infections & Exposures 01-21-22
*Note that isolation timelines (for members with a COVID infection) do not change with vaccination status*
*For work restrictions / Quarantine, only members who are “Up to Date” are exempt from work restrictions under conventional staffing levels.*
*Definition of being “Up to Date” for vaccination can be found HERE*
IDPH News Release 12/30/21
This IDPH release directs EMS agencies to follow CDC’s HCP guidance. “IDPH has already adopted CDC’s updated guidance for health care personnel issued last week. Health care personnel and other specific groups and setting should continue to follow their respective guidance.”
*CMS Update from 12/28/21 about Vaccine Mandate*
As a reminder the CMS vaccine rule does not apply directly to locals providing ambulance services but the rules do require hospitals, nursing homes, CAHs, and SNFs to require COVID-19 vaccines for “individuals who provide care, treatment, or other services for the facility and/or its patients, under contract or by other arrangement.” While CMS mandate does not directly apply to 911-EMS agencies you should prepare to possibly address requests from facilities to provide vaccination information.
What PPE should I wear?
Please consult the CDC recommendations, found HERE.
How should I don / doff my PPE?
Please consult this VIDEO provided by the CDC.
What is the difference between quarantine and isolation?
Quarantine is remaining at home or another identified location with little to no public interaction due to exposure to a known COVID-19 patient, but the quarantined member isn’t having signs of infection. Isolation is a mandated situation due to a member exhibiting signs and symptoms of infection.
Who is in charge of forcing quarantine?
In Illinois,The Department of Public Health has supreme authority over declaring new or modifying existing quarantines. A county board of health should be created with responsibility for control of contagious diseases, including the use of quarantine for areas within the county not incorporated. Corporate authorities of municipalities have jurisdiction for quarantine extending one-half mile beyond corporate limits. Local health authorities shall establish quarantine of contacts of someone suspected of carrying a disease that requires this action.. that law is found here Public Health Act
When should our members get tested for the virus?
Please consult the CDC guide found here, CDC Guide also, any of our members traveling from high risk level 3 areas should strongly consider a 14 day self quarantine.
Where should our members be quarantined?
Home quarantine is acceptable, except if the member will be around immune-compromised or elderly household members. Also, if the member cannot maintain a 6′-10’ distance from family members, alternative locations need to be considered. Many of our departments locally, and nationwide have identified one station as a quarantine spot.
How should we approach suspected infected patients?
The best advice, for conservative use of PPE supplies, and to minimize the amount of members that could suffer an exposure, Best treatment strategies for suspected COVID-19 patients;
If a patient exhibits cough, fever, or has traveled from high risk areas you should;
1. Put one EMS worker in full PPE as described above. All others should avoid Pt. contact. That one fully dressed member should immediately have the patient place a facemask on the patient and instruct the patient to walk outside to the door or ambulance.
2. In the event any aerosolizing interventions are required (such as CPAP, intubation, suctioning, BVM, etc.) all EMS providers within 6’ of the patient or inside the patient compartment of the ambulance must have full airborne precautions in place (N95 respirator or higher, gown, eye protection or face shield, and disposable gloves).
3. If you are fully dressed as described, at this time the CDC is not considering that exposure due to proper PPE in place.
4. Assure your department has communicated with your local hospital(s) on what the arrive plan is at the ER.
What disinfectant should be used to decon?
The EPA provides this guidance for what to look for in a disinfectant “ The product is an EPA-registered, hospital /healthcare or broad-spectrum disinfectant with directions for use on hard, porous or non-porous surfaces2.”
A complete list of approved Coronavirus disinfectants is found HERE.